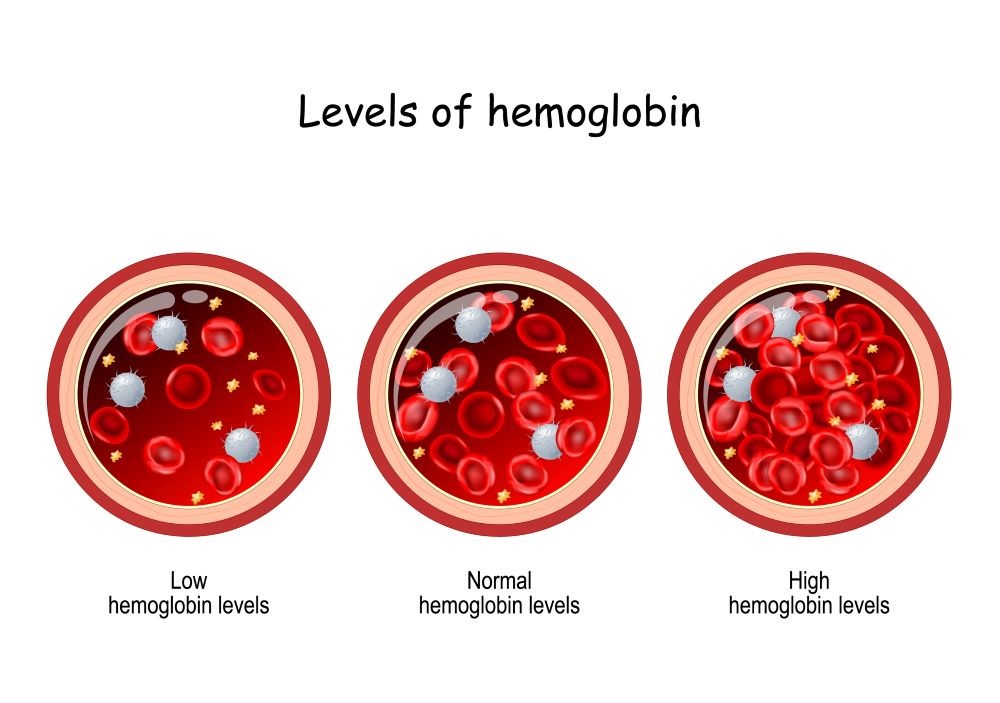
Pregnant Women & Hemoglobin Levels:
(Ways to Up Your Platelet Count Naturally)
Red blood cells (RBC) are in charge of carrying oxygen throughout the human body. Hemoglobin is a protein found in these cells. This hemoglobin aids red blood cells in storing and transporting oxygen to various regions of the human body. This protein also aids in the movement of carbon dioxide from various areas of the human body to the lungs, where it is expelled.
To synthesize RBC and hemoglobin, the human body requires a steady supply of critical nutrients such as iron and many vitamins. Anemia can result from a decline in hemoglobin levels. When there is insufficient oxygen supply, the human body ceases to operate correctly.
- The ideal hemoglobin level for pregnant women is between 11 and 16 g/DL. In the first and third trimesters of pregnancy.
- Hemoglobin levels should be higher than 11 g/DL. In the second trimester of pregnancy.
- Hemoglobin levels should be higher than 10.5 g/DL. A pregnant lady is deemed anemic if her hemoglobin level goes below 11 g/DL.
- There are various natural strategies to boost hemoglobin levels.
# Low Hemoglobin Level Cause? (In Pregnant Women):
When the human body does not receive the necessary amount of critical nutrients such as iron, the hemoglobin level of a pregnant woman can decrease—the volume of blood in the human body grows during pregnancy.
As a result, the body of a pregnant woman would require an extra amount of iron (beyond the regular demand) to synthesize more RBC. Anemia can be caused by a lack of iron,
However, the illness is not life-threatening unless and until the RBC level drops abnormally.
(Pregnant women’s hemoglobin levels can drop as their newborns use the RBC stored in their moms for development and growth.)
The following conditions increase the likelihood of acquiring anemia.
- If pregnant with multiple babies
- If Daily diet does not contain the recommended quantity of iron for expectant moms
- Getting pregnant multiple times in a short period
- If the pregnant mother had a heavy flow of blood during her menstrual cycles prior to pregnancy
- If the expecting mother vomits regularly due to morning sickness
Choose natural methods to boost hemoglobin count or visit a Gynecologist doctor to enhance a pregnant woman’s hemoglobin level with appropriate and dependable medication.
Symptoms:
In a pregnant woman, a modestly low hemoglobin level does not cause noticeable symptoms.
Only if there is a decline in hemoglobin is substantial and highly abnormal can symptoms appear.
If the following symptoms persist, you should see a doctor:
- Pale skin, palms, the underside of eyes, nails, lips. etc
- Constant exhaustion and tiredness.
- Recurring dizziness or vertigo
- Labored or shorter breathing
- Rapid heartbeat
- Difficulty focusing
# Risks of a Low Hemoglobin level:
• Premature or underweight babies after Pregnancy Delivery.
• Excessive blood loss during labor
• Postpartum depression.
• Anemia can be present at birth.
• Babies can experience developmental delays.
# Ways to Increase Hemoglobin level naturally:
Consuming foods high in iron is one of the most commonly recommended natural strategies to boost hemoglobin levels.
- Fruits and leafy vegetables rich in hemoglobin include:
(Spinach, tomatoes, parsley, green peppers, Brussels sprouts, cabbage, turnips, asparagus, peas, kale, broccoli, figs, oranges, apricots, and apples.)
- Some Dry Fruits to eat for low hemoglobin include:
(raisins, hazelnuts, peanuts, dry figs, dates, and almonds.)
- Wheat, cereals, oats, and barley are among of the finest foods for hemoglobin since they are high in iron.
- Non-Veg to eat for low hemoglobin include:
(Chicken, lamb, cattle, hog, liver, oysters, prawns, sardines, tuna, clams and eggs.)
Other natural ways to boost hemoglobin levels include increasing vitamin C intake, which aids in iron absorption from the diet.
- Items high in Vitamin C, such as:
(cauliflower, potatoes, green pepper, tomato juice, cantaloupe, kiwis, and strawberries) are also good in hemoglobin.
Doctors typically give iron supplements to pregnant women based on a variety of factors such as hemoglobin level, food plans, and the stage of the confirmed pregnancy.
Normally, iron supplements can be taken orally, but if the mother is unable to tolerate them, the minerals are supplied intravenously.
If pregnant women are advised to take iron supplements, they should avoid foods that inhibit iron absorption. Cheese, wine, yoghurt, coffee, ice cream, tea, and milk all inhibit iron absorption.
As a result, it is preferable to take these foods a few hours after taking iron supplements.
To maintain healthy hemoglobin levels throughout the pregnancy, consume the best foods for hemoglobin in suitable portions!
# FAQs:
1. What is a pregnant woman’s standard hemoglobin level?
A pregnant woman’s hemoglobin level should be between 10.5 g/DL and 13 g/DL. When hemoglobin dips below 11 g/DL, it is necessary to visit a doctor.
2. Is a hemoglobin level of 9.3 normal during pregnancy?
No, pregnant women with this hemoglobin level should see their doctor right away to avoid pregnancy issues.
3. Is 8.5 hemoglobin considered normal during pregnancy?
No. This hemoglobin level is abnormally low in pregnant women. This level might commonly make mothers dizzy and exhausted.
4. Is a hemoglobin level of 9.7 normal during pregnancy?
No. A hemoglobin level of less than 10.6 g/DL is considered low. This hemoglobin level might cause a number of health issues for both the mother and the baby.
5. What is a low hemoglobin level in pregnancy?
A hemoglobin level of less than 10.5 g/DL is considered low in pregnant women. If your hemoglobin level falls below 5 g/DL, you should see a doctor right away. It takes 6-12 weeks to restore abnormally low hemoglobin levels to normal levels.
6. What foods should you eat if you have low met hemoglobin?
A nutritious diet is one of the most effective natural strategies to enhance hemoglobin count. Iron-rich foods are the best for hemoglobin production. Foods to eat for low hemoglobin include lean meat, plant-based iron-rich foods, fruits and vegetables high in Vitamin C, and so on.
Book an online appointment with Dr. Pooja Vyas Bansal for Pregnancy & gynecology related issues